If untreated, diabetes is associated with a multitude of complications leading to increased morbidities and mortality. Still, nearly half of the people with diabetes are undiagnosed.
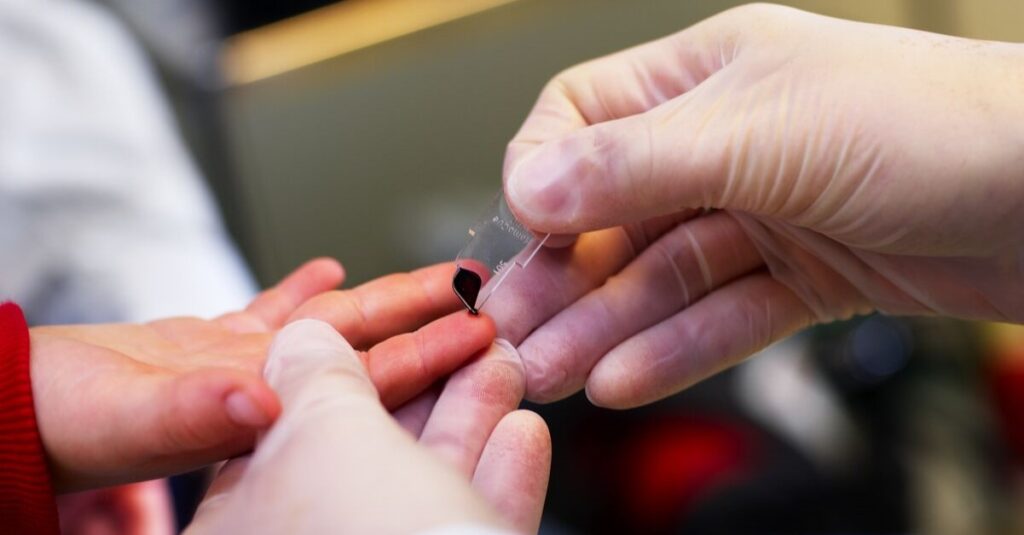
Early detection is crucial in preventing or delaying long-term health complications, potentially saving lives. However, success in screening for or aiding in diagnosing diabetes depends on accurate blood glucose measurement. Equally, screening diabetic patients is needed to properly manage the condition.
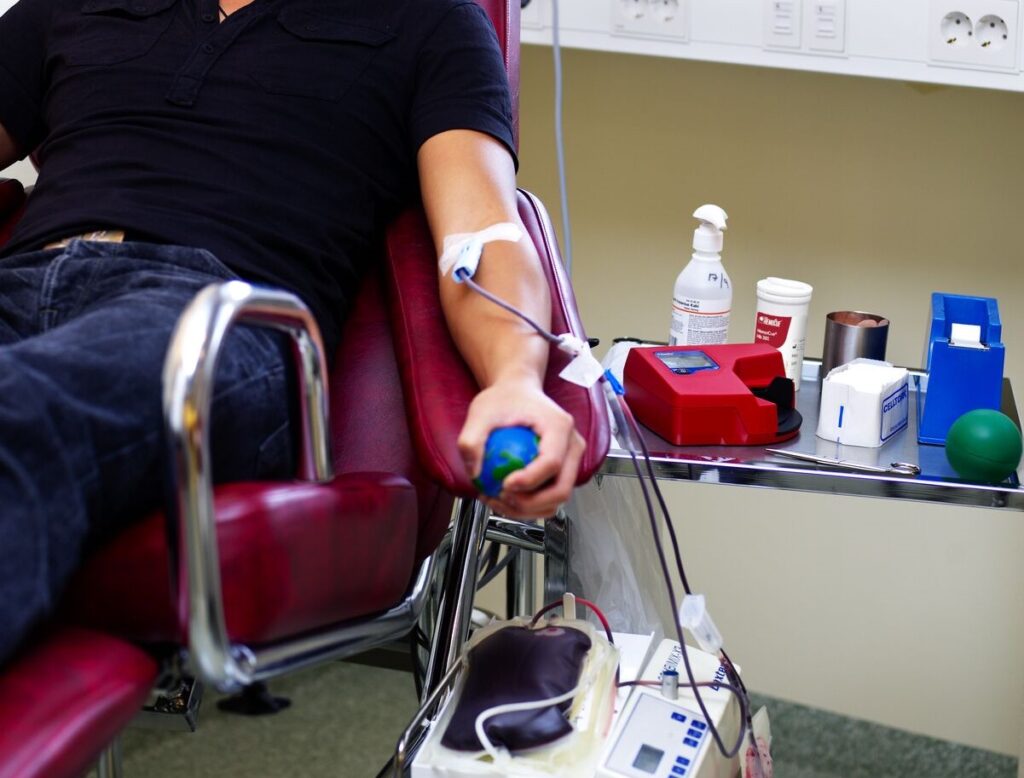
HemoCue offers tools that provide accurate testing at the point of care for diabetes and glucose management. Our systems can be used in screening, monitoring, and as an aid in diagnosing diabetes type 1, type 2, and gestational diabetes.
Learn more about diabetes at our Knowledge Center.